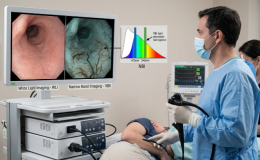
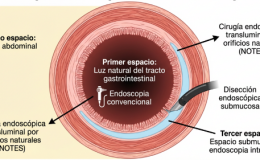
The past decade has seen a paradigm shift in our understanding of the brain-gut axis. The exponential growth of evidence detailing the bidirectional interactions between the gut microbiome and the brain supports a comprehensive model that integrates the central nervous, gastrointestinal, and immune systems with this newly discovered organ. The brain can affect the community structure and function of the gut microbiota through the autonomic nervous system, by modulating regional gut motility, intestinal transit and secretion, and gut permeability, and potentially through the luminal secretion of hormones that directly modulate microbial gene expression.
Brain-Gut Axis
The enteric nervous system (ENS) consists of more than 100 million neurons that are organized into highly complex microcircuits that can function independent from the central nervous system (CNS) and spinal cord. ENS communication with the CNS is continuous and bidirectional. The gut and the brain communicate via the parasympathetic nervous system through efferent motor pathways of the vagus nerve and via the sympathetic nervous system through efferent motor pathways of the prevertebral ganglia.
Abnormalities in brain-gut communication are one way that brain-gut axis disease may arise
Every class of neurotransmitter found in the CNS is also detected in the ENS
Brain-Gut-Microbiota Axis
The brain-gut-microbiota axis is modulated by the enteric microbiota. Gut microbes communicate to the CNS through at least 3 parallel and interacting channels involving nervous, endocrine, and immune signaling mechanisms. The microbiota can modulate the CNS directly via the vagus nerve and/or indirectly by influencing the ENS and by production of metabolites that cross the blood brain barrier. Serotonin is important for brain-gut communication as both a neurotransmitter in the ENS and CNS, as well as a hormone present throughout the circulation.
Hypothalamic-pituitary-adrenal axis
The hypothalamic-pituitary-adrenal axis (HPA) is part of the limbic system (brain area involved in emotional responses). HPA axis activation can be initiated by stressors and/or systemic proinflammatory cytokines that induce secretion of corticotropin-releasing factor (CRF) from the hypothalamus. CRF secretion stimulates stimulates adrenocorticotropic hormone secretion from the pituitary gland that leads to cortisol release from the adrenal glands.
Serotonin
There is significant evidence to suggest that serotonin may be an important link in the brain-gut axis. Serotonin and its primary inactivator, the serotonin reuptake transporter, are present in both CNS and the ENS where they are critical mediators of development and function. The vast majority of serotonin (approximately 95%) is found in the intestine. Approximately 90% of enteric serotonin is located in the intestinal epithelium, in enterochromaffin cells, with the remainder located in neurons of the ENS.
Current evidence indicates that bottom-up modulation of the CNS by the microbiome occurs primarily through neuroimmune and neuroendocrine mechanisms, often involving the vagus nerve
This communication is mediated by several microbially derived molecules that include short-chain fatty acids (SCFAs), secondary bile acids(2BAs), and tryptophan metabolites. These molecules propagate signals primarily through interaction with enteroendocrine cells (EECs), enterochromaffin cells (ECCs), and the mucosal immune system, but some cross the intestinal barrier, enter systemic circulation, and may cross the blood-brain barrier. The microbiota can independently produce or contribute to the production of a number of neuroactive molecules, including but not limited to serotonin,dopamine, norepinephrine and gamma-aminobutyric acid.It remains poorly understood if these molecules reach brain sites directly or only induce central responses via long-distance neural signaling.
There are at least 12 different types of these cells with several subtypes (in particular A,K and L cells) present as subgroups along the intestine that contain different combinations of molecules. ECCs are interspersed between gut epithelial cells throughout the length of the gut and contain more than 20 different types of signaling molecules, which often are colocalized and co-released. Released in response to chemical and or mechanical stimuli, these molecules can enter the systemic circulation and reach centers in the CNS involve in ingestive behavior (nucleus tractus solitarius and the hypothalamus) or act locally and activate closely adjacent afferent vagal terminals in the gut or liver to generate brain signals.
SCFAs have been implicated as major signaling molecules mediating host-microbiome communication via EECs and ECCs. These molecules are generated by microbial fermentation of host dietary-resistant starch and nonstarch polysaccharides and serve an important part in the host energy harvest while also stimulating colonic blood flow, fluid and electrolyte uptake, and mucosal proliferation. Dietary fiber intake is a major regulator of SCFA concentrations. One of the best characterized examples of these microbial host interactions is the bidirectional interaction between microbes, ECCs, and the CNS. Serotonin has a central role in regulating GI motility and secretion, there is likely immense selective pressure on the gut microorganisms to act on the serotonergic system to modulate their environment effectively (regional transit times and fluid secretions). SCFAs and 2BAs derived from spore-forming bacteria of the gut regulate a significant percentage of ECC serotonin (5HT) synthesis and release.
The essential amino acid tryptophan (Trp) is a key molecule in the BGM axis because it is the precursor to serotonin and a number of other metabolites that contribute to the neuroendocrine signaling. Gut microbiota contribute to the peripheral availability of Trp which is imperative to the CNS synthesis of serotonin.