The intestinal epithelial layer forms the major barrier that separates our body from the external environment. Trillions of commensal bacteria reside in the gastrointestinal tract and have a vital role in digestion and the development of the immune system. The maintenance of the intestinal epithelial barrier is the essential function of the intestinal epithelial cells (IECs). The mucosal protective barrier is a feature of higher animals and has been developed and maintained throughout evolution. The family of mucus glycoproteins, the mucins, are an integral part of this barrier. The mucus layer provides a niche for bacterial colonization because it contains attachment sites and is also a carbon source.
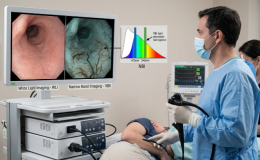
The gastrointestinal mucosa has the complex task to act as a semipermeable barrier that allows the absorption of nutrients and immune sensing,while limiting the transport of potentially harmful antigens and microorganisms. The epithelial layer is composed of a simple monolayer of around 20 billion contiguous cells, which,like the skin,continually regenerates.
Stem cells, located at the base of the crypts of Lieberkuhn, produce daughter cells that differentiate. As the progeny cells migrate toward the luminal surface, they lose their proliferative capacity and differentiate into specialized cells, which include colonocytes and mucin producing goblet cells. Cells at the luminal surface eventually undergo programmed cell death (apoptosis) and are shed. From birth to death,the regenerative process is complete within a few days.Mature cells facing the lumen (surface cells)are in close apposition to layers of mucus.The cells and the mucus together form a layered barrier separating the body from the colonic microflora and limiting influx of bacteria and bacterial antigens. The combination of the epithelial sheet and the mucus layer forms a biologically flexible and environmentally responsive barrier to luminal contents.
In the large intestine, where is nothing resembling Paneth cells that secrete antimicrobials, physical barriers mainly contribute to spatial segregation of gut microbiota and intestinal epithelia. Physical barriers consist of the mucus layer covering the intestinal mucosa, the glycocalyx on the microvilli of absorptive ICs, and the cells junctions firmly linking IECs. These barriers physically inhibit the microbial invasion of the mucosa.
The colonic mucosa secretes copious amounts of mucus, which is composed of complex and extensive O-linked oligosaccharide modifications on a mucin protein back-bone.These glycoproteins form large disulfide-linked macromolecules,and upon release from goblet cell granules into the lumen,become hydrated and expand to form a net-like gel.
The small intestine contains a single layer of loose unattached mucus, mucus in the colon is organized into three distinct layers.
The inner mucus layer is stratified and anchored to the intestinal epithelia, which does not allow gut bacteria to easily penetrate into the inner mucus layer and thereby keeps the inner mucus layer free of bacteria. The inner mucus layer is converted into the outer mucus layer by the proteolytic processing of polymerized MUC2 by the host or gut bacteria.
The absence of dietary fiber, a major energy source of intestinal bacteria, leads to the expansion of mucin-degrading species, resulting in the increase of inner mucus degradation
The adherent mucus is synthetized and secreted by the Goblet cells, located in all parts of the intestinal tract.The function of the goblet cells vary depending on their location in the small intestinal or colorectal crypts. The family of mucin genes currently includes 21 members.They have been divided into two basic groups on the basis of their biologicals functions, secreted mucins and the membrane-associated mucins.
In the small and large intestine, mucin 2 (MUC2) is the most abundant mucus protein secreted by goblet cells. Membrane-anchored mucins associated with the colonic epithelial cells form the glycocalyx. The glycocalyx gives way to a second tightly crosslinked inner layer composed of the mucin protein MUC2. The outermost layer,generated by proteolysis of the inner layer, is less dense and less viscous.The outer layer of colonic mucus is the habitat for both indigenous and transient microorganisms, called autochthonous and allochthonous, respectively. Mucus provides nutrients to bacteria, including amino acids and sugars, which are especially important for those bacteria capable of degrading the glycans on the mucin backbone.
The expression of the mucins in the mucosal defensive barrier is dynamic and is known to adapt to mucosal changes, in order to maintain optimal protection
The mucus layers achieve different densities, such that commensal flora or even pathogens can reside within the low density outer layer but are generally excluded from the high density inner layer and glycocalyx. A second means of separating the bacteria is mucus turnover. As secreted mucus is extruded,proteolyzed in the inner layer, and secreted into the lumen,bound bacteria are expelled and removed from the body by intestinal peristalsis.
The mucus layer is the very first line of physical defence that external molecules encounter when they arrive in the gut lumen, and which prevents bacteria from directly contacting the epithelial cells
Defective mucin production or processing has been linked to inflammatory bowel disease. Ulcerative colitis patients have fewer goblet cells and decrease synthesis and secretion of MUC2, especially during episodes of severe disease.
The gastrointestinal microbiota shows characteristic patterns throughout the tract and this has implications for the nature of interactions between the bacterial cells and the mucosal surface glycoarrays. Oral cavity species include Streptococcus, Prevotella, Porphyromonas, and Fusobacterium strains, stomach accommodates Streptococcus, Lactobacillus, Staphylococcus, and Peptostreptococcus, while an abundance of more than 1000 species are found in the small intestine and colon.These are largely anaerobes, with 2-3 times more than facultative anaerobes and aerobes.
Metabolites from gut bacteria also directly enhance the mucosal barrier function. Mucus secretion from goblet cells is upregulated by butyrate, one of the short-chain fatty acid (SCFA) provided by gut bacteria. Recent evidence revealed that the expression of cell junction-associated molecules such as occludins and claudins in IECs is enhance by indole, a metabolite of dietary tryptophan from commensal bacteria possessing trytophanase.
The ability of the human enteric microbiota to turn over mucus in the intestinal mucosa depends on the production of a series of hydrolytic enzymes, which degrade the mucus glycans to yield monosaccharides which serve as an energy source for the microbiota.
The mucosal barrier function of IECs is also enhanced by cytokines from immune cells activated by gut commensal bacteria or pathogenic bacteria. In the case of Citrobacter rodentium infection associated with enteritis, a potent Th17 cell-mediated response is induced. IL-17 and IL-22 produced by Th17 cells upregulate the secretion of antimicrobial peptides by IECs which work to regulate commensal and pathogenic bacteria.
Role of the Mucus Layer
The mucus barrier has an important role in regulating the severity of infectious diseases. It provides protection against many intestinal pathogens, including Yersinia enterocolitica, Shigella flexneri, Salmonella and Citrobacter rodentium.
An alteration of mucosal integrity is generally associated with health problems, such as inflammatory bowel diseases,including ulcerative colitis and Crohn’s disease.
Mucolytic Bacteria
A distinct subset of intestinal bacteria possesses the enzymatic activity, such as glycosidases,necessary for the degradation of mucin oligosaccharides,wich can be further metabolized by resident microbiota.
Bacterial Adhesion to Mucins
Mucins proteins are highly glycosylated. Their O-glycans are used as ligands for bacterial adhesins.
Bacterial Biofilm and Mucus
There are more mucus-associated bacteria in the proximal region of the colon than in distal colonic sites.
Impaired mucin production is related to colorectal cancer that is also linked to the presence of biofilms
Modulation of mucin composition by bacteria
Different probiotic agents, such as Lactobacillus species, can stimulate the production of MUC2 and thereby the secretion of mucin in the intestine, improving pathogen resistance. Bacterial fermentation products, such as short-chain fatty acids (SCFAs) like butyrate and propionate enhance the production of MUC2 by the goblet cell in the gut.