Biofilms
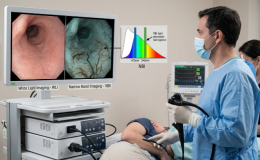
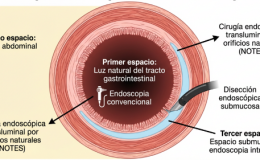
Biofilms are microbial communities embedded within an extracellular matrix, forming a highly organized structure that causes many humans infections. Dental caries is a polymicrobial biofilm disease driven by diet and microbiota-matrix interactions that occur on a solid surface. Periodontal disease is caused when biofilms replace the commensal microflora on the dental plaque surface and promote the chronic inflammatory destruction of periodontal tissue. Many infectious diseases are caused or exacerbated by biofilms. Defining the microbiome in the oral cavity may be far more complex and challenging than initially envisioned,which,in addition to many bacterial species (bacteriome),also harbors fungi (mycobiome), viruses (virome), and even ultra small organisms (candidate phyla radiation group). In the oral cavity, a diet rich in sugar, particularly sucrose, provide a substrate for the production of extracellular polysaccharides, which form the core of the extracellular matrix in cariogenic biofilms. The matrix can trap or sequester a diverse range of substances,including nutrients,metabolites, and quorum-sensing molecules. Enzymes can be retained and stabilized, transforming the matrix into a de facto external digestive system.

The oral cavity is the starting point of the GI tract and is lined by mucosa that covers the lips and the mouth. Dental disease are now viewed as a consequence of a deleterious shift in the balance of the normally stable resident oral microbiome. An altered oral microbiota has been linked with the development of several oral diseases, such as dental caries, periodontal disease, and oral stomatitis. Poor oral health has been linked to head and neck cancer, particularly oral cancer. In particular, about 700 bacterial species have been identified in oral cavity and, more importantly, 35% of them have not been cultured. Ecological imbalance of microbial community (dysbiosis) is characterized by: loss of beneficial microbes, expansion of pathogenic microbes, and general loss of microbial diversity. It is becoming evident that dysbiosis can lead to cancer development. In healthy saliva and oral mucosa, the predominant bacterial phyla consist of Firmicutes, Bacteroidetes, Actinobacteria, Proteobacteria, Fusobacteria, TM7 and Spirochaete. Periodontal diseases are dysbiotic conditions in the gingival margin, which are characterized by an imbalance between subgingival communities and the host immune response. Such diseases include gingivitis, which is a reversible condition characterized by the inflammation of the gingiva driven by the combined effect of specific microbial taxa. If not treated, gingivitis could progress to periodontitis, characterized by the destruction of supporting tissues of the teeth.
Orodigestive cancers are highly influenced by both a direct carcinogenic effect of periodontitis-associated bacteria in either oral cells or in other body sites and inflammatory mediators migrating from the oral cavity. Despite the natural dissemination of oral bacteria due to swallowing of saliva, which contains a large number of bacteria, there is also evidence showing dissemination through the bloodstream. Dental or oral surgery is considered to be predisposing factors for anaerobes bacteremia in both adults and children.
Oral squamous cell carcinoma is the most common type and a major cause of morbidity and mortality. There is an increased presence of saccharolytic and aciduric bacteria in oral cell carcinoma as compared to normal tissue. This suggests the presence of specialized microbes attached by the acidic and hypoxic tumour environment. Differences in bacterial composition of tumour versus normal adjacent tissue included an increased abundance of phylum Firmicutes (85%), and a relative shift of Gram negative to Gram positive microbiota, including saccharolytic Streptococcus. Potential biomarkers of oral squamous cell carcinoma: Prevotella melaninogenica, Capnocytophaga gingivalis and Streptococcus mitis (Sensitivity and specificity ≥ 90%).Oral dysbiosis seem to be more pronounced in patients with tumours of the gastrointestinal tract, in particular esophageal,gastric, pancreatic, and colorectal cancers.
Emerging studies suggest that cancer sites present a loss of richness and diversity of commensal species, and such microbial disturbances may enhance emergence of carcinogenic species or modulation of the inflammation status to indirectly promote cancer development
It is not the colonization of specific bacteria what triggers the disease, but rather changes in the relative abundances of specific taxa in the subgingival communities due to dysbiotic processes. Ecological catastrophe establishes that the environment and host factors, such as poor hygiene, inappropriate diets, and use of tobacco and drugs produce site effects in the immune defence of the patient